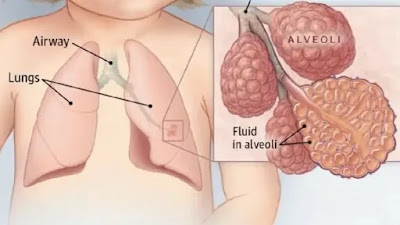
Cervical cancer
Why. cervical cancer is the most common cancer in women in
developing countries and is curable if detected early. Targeted screening for
cervical cancer is highly recommended within a primary health care strategy
when the capacity exists, preferably at the district level, for reaching the
women at highest risk. Targeted screening and treatment should be combined with
action for primary prevention through the provision of access to safe family
planning methods, the prevention and control of STD , and the prevention of
smoking which is an important risk factor for cervical carcinoma. the woman at
highest risk are those over 35 years of age and those with STDs.
Who, how , and when. Who has developed recommendations for
cervical caner screening that are relevant to the needs of developing countries
(WHO meeting, 1986; Stanley et al , 1987; stjernsward et al , 1987). WHO
collaborating centres have made important contributions in that area (habbema,
1990). The following comments are a summary of those findings.
A phased –in approach is rational wherever shortage of
resources makes it impossible to cover all women at risk with screening through
pap smears at suitable intervals. One of the key limiting factors in many
countries will be the number of trained cytotechnicians orcytotechnolgists
available to read smears accurately. First, every women should have a pap smear
once between the ages of 35 and 40. When more resources are available the
frequency of screening should be increased to once every five or ten years for
the age groups 35to 55tears and , ideally, once every three years for women
aged between 25 and 60 years ( who MEETING, 1986) . it is worth noting that women over 65 who have
been repeatedly found negative in previous pap smears do not need further
testing (USPSTF,1989)
According to this phased –in approach, priority is given
first to expanding the coverage of women in the age groups at highest risk and
subsequently to increasingly frequent screening of those covered. The coverage
of women aged 35 and over will require a special public education and outreach
effort, because such people are generally not reached by maternal and child
health services . most of the population at risk could be missed if efforts are
concentrated on ante partum and postpartum women , woman bringing their
children for well- child care , and women seeking help with family planning .
It is common practice in many countries to make pap smear
screening a routine component of care for women seen by family planning services.
In planes where the older population is not yet covered and only a limited number of pap smears can be done,
this practice should be reconsidered within the framework of the phased-in
approach described above. The effectiveness
of cervical cancer screening is more likely to be improved by extending
testing to women who are not being screened and by improving the accuracy and
follow- up of pap smears than by frequent re-screening of the same women.
Coverage should not be expanded without a guaranteed
infrastructure to ensure effective follow up (timely return of results to the
responsible care provider and to the patient), definitive diagnosis , and
treatment. Treatment should be made available as close to home as possible,
since some women, especially those with very young children, may refuse
treatment that requires them to leave their families . the treatment offered
should include curative treatment when possible; where cure is not possible, it
should include effective palliative therapy to relieve pain.
The option of using visual examination instead of cytology
as the initial screening technique has been suggested as worth exploring in
places where resources are particularly scarce (stjernsward et al., 1987;
luthra et al ., 1988; miller, 1992). Under this option , primary care workers
or auxiliaries are trained to carry out a visual examination of the cervix, using a speculum and without
taking a specimen for cytology. Cytology is performed only on those at highest
risk because of their history, or those with a suspicious examination or with
symptoms. This approach is known as downstaging , the detection of disease in
an early stage when still curable, by nonmedical health workers. The phased in
approach , based on expanding coverage before increasing screening frequency,
is used , and the public is educated to seek services. However, visual
inspection would miss many cases of dysplasia (garud et al ., 1983;yang et al ,
1985; engineer &misra 1987). The assumption behind the downstaging approach
using visual examination is that , in many cases, the natural history of
cervical carcinoma is relatively slow, and there is thus considerable time
between the appearance of a clinically detectable lesion and the development of
in curable disease (stjernsward et al . 1987;luthra et al , 1988) . this is a
promising approach that requires testing for effectiveness; it is intended for application
where resources are severely limited, which may not be the case in all
developing countries.
Pending results of studies of the use of visual examination
of the cervix as the initial screening technique, another option is ot use the
system of priorities suggested by who studies, and maximize the use of trained
paramedical workers to perform pap smears (sampaio goes et al ,. 1981;luthra et
al ,. 1988). Alternative suggestions are that one cytological regardless of age
(shrivastav et al ,.1986; ayangade &akinyemi, 1989) and that screening
should be repeated every 5 years , especially for those with additional risk
factors (smoking, prior dysplasia or malignancy, a sexually transmitted disease, a number of
male partners, or a single male partner with a number of partners).
Another option, which is clearly preferable if resources
permit, is to perform cytology once on all heterosexually active women aged
20-64 , or with parity greater than tow regardless of age, and to repeat the
screening one year later to rule out false negatives. For women with two normal
smears and no special risks, screening may be repeated every 5-10 years , with
more frequent screening for those with additional risk factors.
Skilled technicians can be trained to do a first reading,
with a pathologist reviewing equivocal or suspicious suspicious smears, and carrying out spot checks of
random samples for quality control . all smears should be sent to a central
laboratory so that the technician can have enough work to maintain a
sufficiently high level of skill ( J stjernsward, personal communication, 1989)
Screening and treatment need to be done in a manner
consonant with cultural values. In most places, this will mean that screening
should be done by women care providers. Attention needs to be paid to the
issues of privacy and confidentiality; this may require a special effort during
training and the organization of services and information systems , when
primary care workers are involved and support of the community for follow-up
action is sought.
At the time of screening there must already be a realistic
plan in place for ensuring that information on the examination or test result
gets back to the women screened, together with support for appropriate follow-up action.such support may
involve community organizations , as in a study in lesothol where village
chiefs helped locate women with abnormal results who did not return for
follow-up (snhneider & meinhardt, 1984;lynch et al ,.1985) and
encouraged them to receive care . the treatment plan need s to take into
account transport difficulties, economic
pressures, and social responsibilities, including child care , that may
hinder appropriate follow-up , especially in rural areas.
Also at the time
screening is initiated, facilities need to be available within or near the
district, at least for carrying out conization for cancer in situ and localized
cancer, and possibly for performing hysterectomy. Ideally, a facility for
radiotherapy should be readily available. Resources should be allocate for
medication to control pain for those with disseminated disease.
Resource levels required. Low or medium for screening by
visual inspection, but the technique requires more validation; high for
cervical cytology; low or medium for palliation of pain with medication; high
for cone biopsy or other surgery or very high if radiation therapy required.
Recommendation on use of screening . screening of high-woman
(aged 35-55,or with high parity, or with history of STD)with cervical cytology
(papanicolaou smear of cervical cells )is recommended as a priority. Recent studies
suggest that , if it is not possible to carry out cytology for allwomen in the
high-risk category, it is advisable to screen initially by visual inspection of
the cervix and carry out cytological testing for suspicious findings. The recommendation
is uncertain regarding cytological screening of low –risk groups. It is not
recommended to carry out frequent cytological screening of low –risk groups
before the high-risk population has been adequately covered. emphasis should be
placed on primary prevention through smoking cessation, family planning, and
prevention and early detection of STDs.
Research priority. Validation of low-cost accurate methods
of screening.